
When one partner snores, the fallout can be more than a strained relationship – it can be a sign of a potentially serious health problem. Can dental professionals save the day?
By Susan Richards
It starts as a nudge for a snoring partner to roll over. Then, the sawing logs lead to a night on the couch. A good night’s sleep improves the quality of life, but interrupted rest can spell trouble for even the happiest couples.
In a study reported by Newsweek, 18% of participants blamed snoring for rifts in their relationship, and 30% reported sleeping in separate rooms due to the noise. Some respondents even cited snoring as one of the reasons for ultimately divorcing.
Additionally, sleep deprivation for one or both people in the relationship can lead to resentment, guilt, arguments, and decreased intimacy, not to mention cognitive issues and a detrimental impact on physical health.
However, frustrated couples may consider consulting a dentist before a marriage counselor.
Identifying Sleep Apnea
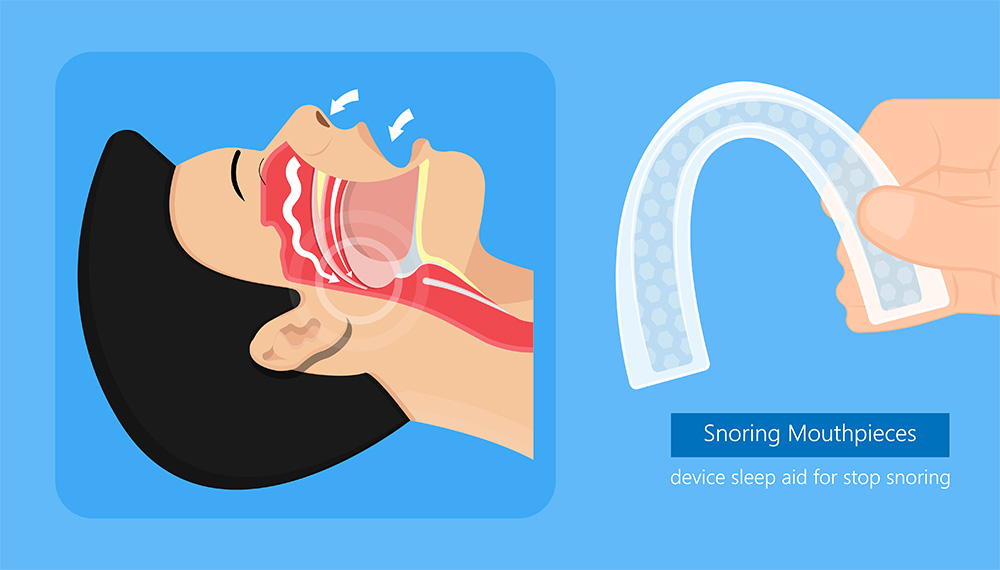
Snoring results from the airflow through the nose and mouth being obstructed for various reasons, including poor muscle tone in the throat and tongue, narrow nasal passages, or enlarged tissue in the throat area. Dentists and medical professionals know to ask about snoring on patient intake because it’s a significant indicator of Obstructive Sleep Apnea – or OSA.
Apnea is a temporary suspension of breath, and OSA is characterized by the American Dental Association (ADA) as a “recurrent narrowing or collapse of the upper airway during sleep, resulting in a partial or complete cessation of airflow.”
According to CPAP.com, sleep apnea is a common sleep disorder that impacts between 50 and 70 million adults in the United States. However, because the symptoms can range from mild to severe, it’s estimated that 75% of sleep-related breathing cases are undiagnosed.
In addition to snoring, some of the signs of OSA that patients and dentists can look for include the following:
- Gasping or choking during sleep
- Morning headaches
- Mouth breathing
- Dry mouth upon waking
- Irregular breathing while asleep – reported by partner
- Enlarged neck, tongue, or tonsils
- Redness in the throat, possibly caused by snoring
- Sleepiness or sluggishness during daytime; inability to concentrate
- Frequent waking in the night to urinate
- Decreased libido
While these symptoms alone may not be concerning, a combination might indicate a sleep disorder.
OSA Signs in the Dental Chair
Because sleep apnea sufferers breathe with their mouths open, they have an increased risk of periodontal disease and gingivitis. Other notable oral health problems, such as dry mouth, tooth decay, sore jaw, and worn-down or sensitive teeth, may indicate a potential sleep disorder, especially when snoring is reported.
A rise in bruxism was noted during the height of the COVID-19 pandemic due to the stress patients were experiencing. But there has been an increased awareness of a possible correlation between bruxism and sleep apnea, the theory being that teeth grinding is an unconscious effort to open the airways.
Studies have also shown that temporomandibular joint (TMJ) disorders and OSA can be related, and patients with two or more sleep apnea symptoms are at much higher risk for TMJ problems.
OSA Risks and Response
Although OSA affects all gender, age, and race demographics, it’s twice as prevalent in men. Those at risk for sleep apnea tend to be male, overweight, over 40, or have a family history of snoring or OSA.
If ignored, numerous potentially significant health consequences of OSA include impaired cognitive function, heart disease, high blood pressure, and depression. CPAP.com reports that 69% of those diagnosed with severe OSA have hypertension, and 70% of rehabilitating stroke patients suffer from severe sleep disorder breathing issues.
Due to these risks, dentists may refer patients with sleep-related symptoms to a primary care physician or sleep medicine specialist who can conduct a sleep study and make an official diagnosis of Obstructive Sleep Apnea.
Breathing Easier
One of the most common treatment options for OSA is continuous positive airway pressure (CPAP) therapy. A machine pumps a steady oxygen flow through a facial mask and into the throat, keeping the airway open all night. While effective, many patients (and their partners) are dissatisfied with the noise and intrusiveness of the CPAP in the long term.
Oral appliance therapy can be a popular treatment modality, either as an alternative to CPAP or in conjunction. Patients can receive a custom-fitted, mandibular advancement device designed to bring the jaw forward slightly, thus preventing the airway from closing, resulting in easier breathing and reduced snoring. Less comfortable but with the same effect on the airway, a tongue-retaining mouthpiece is also available.
The American Academy of Sleep Medicine recommends that qualified dentists provide custom appliances. Patients find the devices convenient, inconspicuous, and easy to care for, and when prescribed for apnea treatment, they’re often covered by insurance.
Mail-order mouthguards – also used for nighttime bruxism or as orthodontic aligners – are less expensive than custom devices. Still, users may deal with more significant oral health issues than snoring if they choose to DIY.
In Conclusion
Not only can dentists play an essential part in identifying the signs of sleep-related breathing disorders like OSA, but potentially serious health issues can be prevented when collaborating with the patient and their physician or specialist.
Perhaps the dentist who can help silence the snoring may also salvage a relationship.
If you're not yet subscribed to receive the Incisor newsletter, filled with cutting-edge dental news sent directly to your inbox twice a month, you can do so here.
Author: Susan Richards is a staff writer at DOCS Education. With over 20 years of experience in local journalism and business marketing, Susan’s career includes award-winning feature writing, as well as creating content with context for a wide variety of industries.




