
Part II: Open Communication is Key
(You can find Part I of this article series, where we discussed oral health implications, here.)
By Timothy Hyland
Marijuana use has been conclusively linked to a number of oral health problems, and the time has come for dentists to engage more openly with their patients about their behaviors, experts say.
Marijuana has long been among the most popular recreational drugs in the United States, but recent trends—including changing attitudes toward the drug and the legalization in many states of medical marijuana—appear to be driving use ever higher. One new study, released on Sept. 15 by the National Institute on Drug Abuse (NIDA), for example, found the percentage of college-age students who confirmed that they used vape-based marijuana in the past 30 days rose from 5.2 percent in 2017 to 14 percent in 2019.
Medical experts and doctors have many different perspectives on the drug’s potential health benefits, but in the world of dentistry, the possible dangers of the legal marijuana to oral health is not yet well-documented. Putting the drug’s therapeutic potential for other health conditions aside, the American Dental Association has found that marijuana use when mixed with tobacco in “street” mixtures is deeply problematic for oral health. Specifically, the ADA says that numerous studies have now concluded that there is a “significantly higher” rate of periodontitis among users vs. non-users, though there is not yet enough study if the effects of commercial grade legal marijuana to know how much of this incidence derives from cannabis or tobacco.
As one 2005 study from an Australian research team concluded: “Cannabis abusers generally have poorer oral health than non-users, with an increased risk of dental caries and periodontal diseases. Cannabis smoke acts as a carcinogen and is associated with dysplastic changes and premalignant lesions within the oral mucosa. Users are also prone to oral infections, possibly due to the immunosuppressive effects.” However, this study was based on illegal marijuana use, not regulated cannabis production which may not be carcinogenic.
Another study, from a team at the Columbia University College of Dental Medicine, linked frequent marijuana use to “higher odds of having severe periodontitis,” while yet another, from researchers at the University of Nevada-Las Vegas, School of Dental Medicine, found that marijuana use among adolescents was linked to even more negative outcomes on dental health than tobacco use. However, neither study considers nicotine found in illegal marijuana as a variable and therefore cannot conclusively expose links between marijuana legally regulated marijuana and oral health issues.
Given these possible dangers, and marijuana’s impact as a sedative on sedated patients, there is rising sentiment among medical experts that dentists can better serve their patients if they take steps to screen for marijuana use.
The Importance of Screening
And as with other societal health challenges—including such difficult issues as domestic abuse and other violence—dentists can play an important role in identifying potentially dangerous behaviors or problematic individual circumstances.

Writing in the journal Addiction in 2015 about substance abuse beyond marijuana alone, for example, one research team concluded that, “the dental setting is increasingly recognized as an untapped venue for the delivery of medical screenings, given the long-term nature and frequent contacts associated with the patient-dentist relationship. Previous research has shown that substance misuse was common in adults seeking dental treatment and that dental practitioners do provide care to a significant number of misusers.”
Of course, in order to play that role—and to get a fuller understanding of their patients’ overall health—they must actively seek to do so. Even as the research team from Addiction pointed to the important role dentists can play in identifying substance abuse, they also concluded that a great many dentists were not comfortable playing intervening when confronted with a patient who was showing signs of drug use, or simply didn’t believe it was part of their job.
“The results of our national representative survey of U.S. dentists indicate that the majority use patient health history forms that include questions about [both legal and illegal] substance [use.] Yet, almost one-half of dentists did not agree that such screening should be part of their professional role. These findings underscore a significant barrier in dentists’ attitudes that may limit the potential of the dental venue to play a role in screening for substance misuse.”
More widespread use of training programs for dentists and their staff, the team recommended, could help turn the tide and make dental offices a more critical link in identifying users of marijuana and other drugs, and could ultimately make for more safe treatment for both dental staff and patients alike.
Caring for Users
Even for dentists or hygienists who may be untrained in the practice of screening for drug use, there are a few simple ways to ascertain whether a patient is an active user of marijuana—and if they are high during the time of a visit.
According to the ADA, a patient who is high may exhibit any number of common behaviors and symptoms, including euphoria, hyperactivity, tachycardia, paranoia, delusions and hallucinations. If and when dentists are confronted with patients exhibiting these behaviors, it’s essential that they take care in their next steps, as the ADA notes:
Increased anxiety, paranoia and hyperactivity may heighten the stress experience of a dental visit. Increased heart rate and other cardiorespiratory effects of cannabis make the use of epinephrine in local anesthetics (for procedural pain control) potentially life-threatening. Patients may be unwilling to self-report marijuana use or unable to answer reliably, but determination of intoxication may be possible during the routine cardiac risk assessment. It is because of the dangers of administering epinephrine or products containing alcohol to a “high” patient, in addition to increased anxiety and paranoia, that dentists may refuse to treat the intoxicated patient, or consider postponing non-emergency treatment for at least 24 hours.29 Additionally, there may be legal implications regarding validity of informed consent with intoxicated patients, especially with irreversible procedures like extractions.
Additionally, there is added consideration in the treatment of active marijuana users who may need anesthesia during treatment--an issue of particular concern, of course, for dentists practicing sedation dentistry. A study published in the May 2019 issue of the Journal of the American Osteopathic Association found that frequent users of marijuana may need more anesthesia than patients who don’t use the drug as frequent users of either a stimulant or a sedative may have built a tolerance. That study eventually led Delta Dental to put out a statement this past spring encouraging patients to be open with their dentists about their marijuana use. The company has since called for more research into the issue.
“Ultimately, more information is needed to determine the overall health and medical implications of marijuana use,” the company said. “Research in this area is hard to come by, because the federal government still considers the marijuana plant a Schedule-1 drug. According to the Drug Enforcement Agency, Schedule-1 drugs are ‘drugs with no currently accepted medical use and a high potential for abuse.’ Because of this limitation, health providers are left to monitor the impact of marijuana on anesthesia, lung health, and tolerance to pain medications in their practices.”
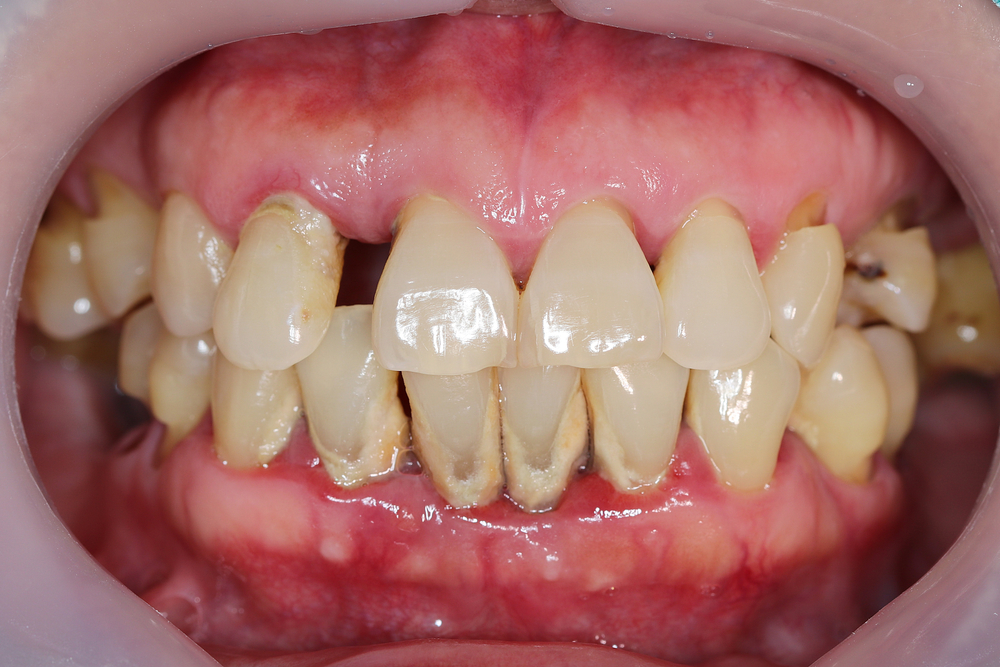
As for patients who are frequent users of marijuana but sober during their visit, there are a number of signs as well, including the following:
- Xerostomia
- Leukoplakia
- Periodontitis
- Gingival enlargement/hyperplasia
- Increased decayed, missing or filled teeth
- Stomatitis
- Candidiasis
- Alveolar bone loss
Both the ADA and a number of studies agree that dentists who suspect a patient may be using marijuana, or any other illegal drug, should engage in a frank discussion about the risks of such behaviors, and the potential health implications going forward.
“If the patient appears to be a user, it may be helpful to understand whether the use is medicinal, as this may suggest relevant comorbidities,” the ADA states in its official guidance to dentists when treating suspected marijuana users. “Verification of cannabis use may be an opportunity to discuss other health consequences and inform the patient of the importance of fluoride, good oral hygiene practices, and healthy snacking.”
Author: Contributing writer Timothy Hyland has more than 20 years' experience as a writer, reporter, and editor. His work has also appeared in Fast Company, Roll Call, Philadelphia Business Journal, and The Washington Times.




