Editor’s Note: Incisor is kicking off a series of dental case studies aimed at giving our readers a virtual tour of specific conditions and treatments, as well as their results.
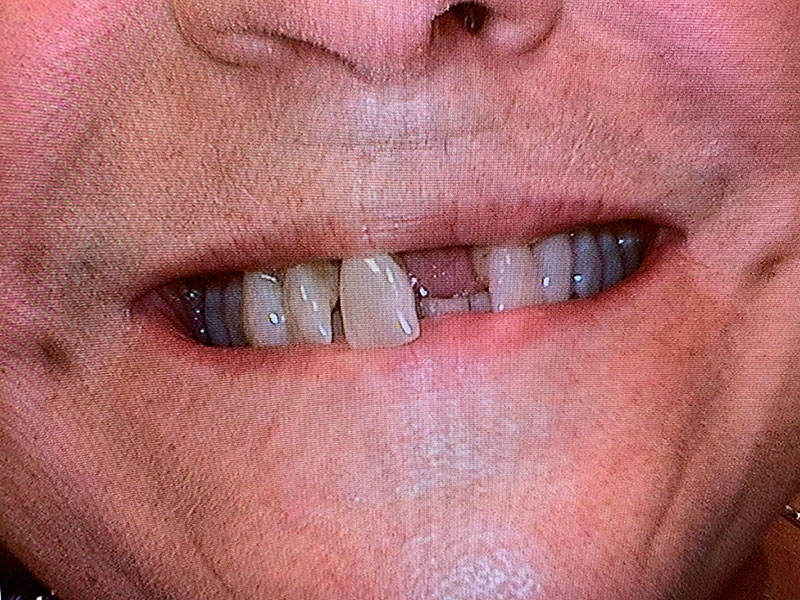
Before
The patient is a 59-year-old female who is on anxiety medication and has panic attacks. She also has thyroid disease, fibromyalgia, high blood pressure, and a sulfa allergy. The patient has not been to a dentist in 8-10 years and her former dentist informed her she was a Bruxer. She does see her physician on a yearly basis and takes Zoloft, Synthroid, a calcium channel blocker, hydrochlorothiazide, and a multivitamin. A patient we had done a full-mouth restoration on referred her, and her friend “absolutely loved our office and results.” She also knew we did oral conscious sedation as she is terrified of the dentist.
The patient came in on an emergency appointment as she had class II mobility on #7 and #10 with class III mobility on teeth #8 and #9. She had no other teeth with any mobility, and she had no acute physical trauma to her front teeth. Interestingly, she knew from her previous provider she was a Bruxer but never acquired or wore an occlusal guard. She also never came back into her previous dentist’s office for any treatment as she was “too afraid” of the dentist. She allowed us to take three pa x-rays, 4 bitewing x-rays, and a panoramic x-ray. We were able to ascertain her immediate concerns but were unable to finish her exam as the fear factor took over. We offered to sedate her for her next appointment, but she declined and was scheduled for the following week. The patient missed this appointment and we followed up with a phone call. She was rescheduled for the following week.
The patient returned three weeks later on an emergency visit after tooth #8 “fell out” while she was eating. She allowed us to finish her comprehensive exam and treatment options. The patient was “desperate” to have something done ASAP as she no longer had a front tooth.
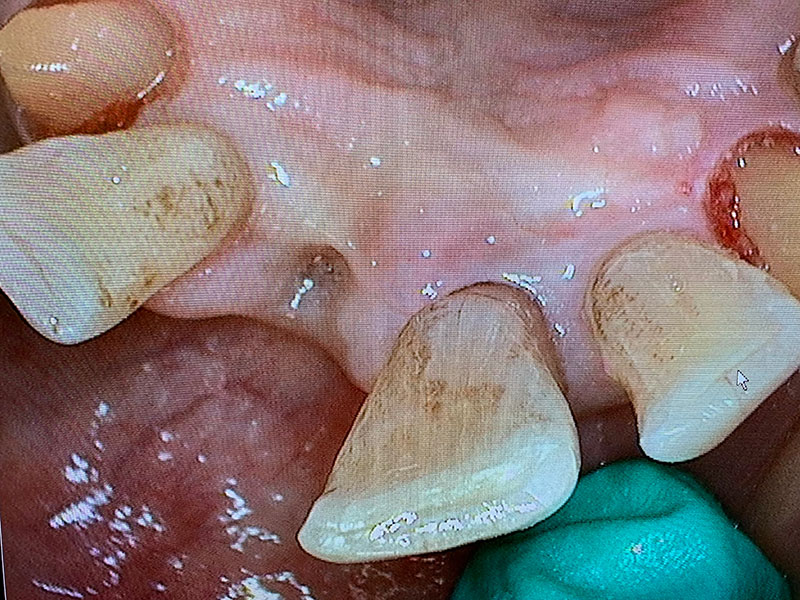
Before
The patient’s diagnosis was a parafunctional habit with tongue thrust and bruxism. She is an ASA II with an Sp02 of 98%. The patient was overweight and her high blood pressure was under control with a baseline blood pressure of 130/82, pulse 78. The patient was a Mallampati III and indicated she snores at night. The patient denied wearing a snore guard or using a CPAP machine.
Our treatment plan consisted of oral conscious sedation with 10 mg of Diazepam the night before the appointment having the patient cease her Zoloft the day of surgery with extractions of #7, #8, #9, and #10,, bone grafting #7, #8, #9, and #10 with cancellous particulate allograft, and doing a 6 unit bridge #6-#11. The patient also understood she would need an upper occlusal guard. Patient was not interested in doing implants as she wanted results quickly and did not want to wear a flipper. She did have other treatment needs but was only concerned with her front upper anterior teeth. She also was quite leery of waiting a year for the final results. She was given the option of a Partial Upper Denture as well but refused this option, not wanting anything removable. The patient ultimately agreed to the six-unit bridge with bone grafting using oral conscious sedation.
The patient signed and dated informed consents for oral conscious sedation, crown and bridge #6-#11, extractions of #7, #8, #9, and #10 as well as allograft bone grafting #7, #8, #9, and #10 on the day she came in for the emergency.
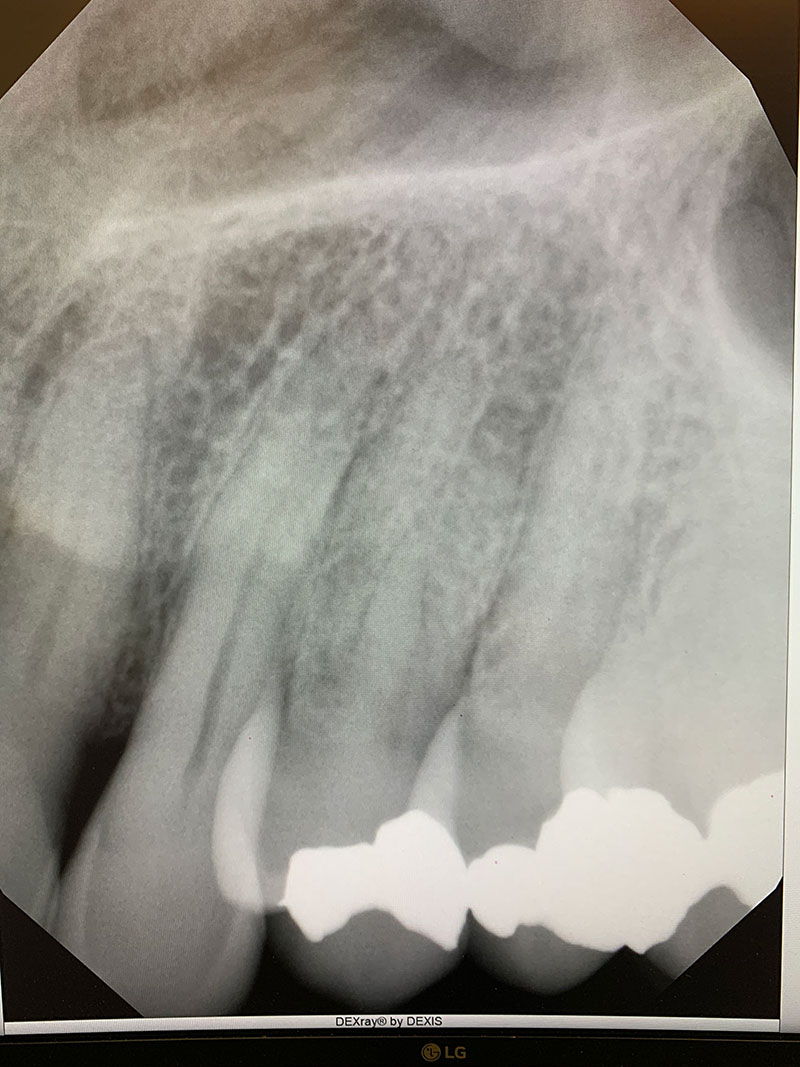
X-ray Before
My informed consents are on separate pages so there is no one-size-fits-all informed consents. As an expert witness in over 150 malpractice cases throughout the unit states, I suggest you would be wise to separate your informed consents and have the patient sign one for each procedure. If the patient just checks a box or signs one blanket consent, it is difficult to defend these cases since the patient can claim she was just handed something and she signed it. If the patient has separate informed consents, their argument is generally moot; they had ample opportunity to ask questions for each informed consent as a separate procedure with the procedure clearly marked at the top in bold large lettering. This method works best. The informed consents must be done before the actual sedation appointment, as they cannot sign any legal documents while under the influence of sedation medications.
Furthermore, the patient understood she would have a large bony defect if no bone grafting was done. Implants placed in this region would work. However, the gum line was not ideal and she was not interested in going through multiple surgeries. The patient also had reservations about implants success. Several of her friends had implants that “failed” or did not have ideal esthetic results even though they were done by specialists in the valley. Given the patient’s concerns, the treatment plan for a six-unit immediate bridge with extractions, bone grafting, and oral conscious sedation fit her needs.
The protocol for oral conscious sedation included 10 mg of Valium taken at bedtime the night before discontinuing her Zoloft for the day of surgery. (The patient takes Zoloft in the morning and we do not allow any anxiety medication the patient normally takes to be taken the day of surgery or allow the patient’s anxiety medication the night before.) We use Diazepam, as it is a predictable drug—we know its half-life, and how it reacts with our oral conscious sedation medications. Generally, we use 5 mg of diazepam the night before, but with any patients that normally take anxiety medication, we generally use 10 mg of Diazepam the night before so they can sleep. We also have adults under the age of 65 years take 0.25 mg of Triazolam one hour prior to the appointment (unless they are hyper responders, in which case, we decrease the dose). It is generally wise to have the patient in your office within 30 minutes of them taking this medication, as the effects can make it difficult for them to walk and you want to be able to assist them if needed. It also allows the patient to be evaluated before the first-pass effect is at its peak. Some offices have the patient take the medication once they arrive in the office. However, it seems more difficult to get the patient in the door without some effect of the drug.
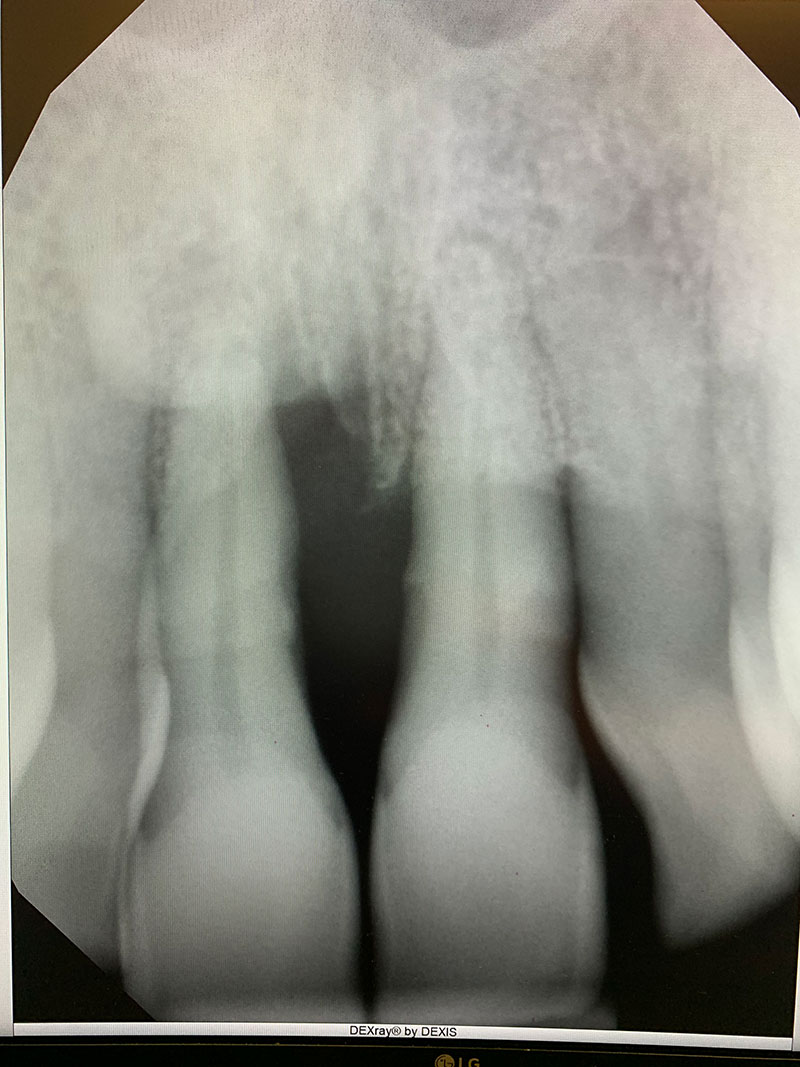
X-ray Before
The patient was sedated at minimum oral conscious sedation when she arrived. We placed her on capnography, and at the one-hour post triazolam mark, we evaluated the patient for the responsiveness. Our patient was mildly sedated and we administered .25 mg of Triazolam sublingual. Within 20 minutes the patient was comfortable enough to begin the procedure. We placed the patient on 02 for three minutes then on N20/02 titrating up to 35% N20/02 for the local anesthetic administration. Once local anesthetic was administered, we placed the patient on 100% 02 for the rest of the appointment, taking blood pressure every 5 minutes. Postoperatively, we make sure the patient is orientated X3 with purposeful movement before discharging them, and we use a companion chair to take the patient to their vehicle. Every time!
The patient was given 875 mg Amoxicillin b.i.d. one day prior to surgery as compliance with this dosage is always better. We also have the patient take the medication at least one day post-operative for any severe periodontal disease/bone loss case in which we have a 10 mm periodontal pocket to deal with. Generally, this eliminates any post-operative infections with our bone grafts and extractions. Elimination of any antibiotics prior to extractions and bone grafting will generally lead to a much higher infection rate and bone graft failure. When doing larger extraction cases, we will give Decadron or a Medrol pack as well. Large extraction cases with implant placement and bone grafting require a higher level of learning and patient management. This case did not require this level of patient management but did require pre-operative and post-operative antibiotic usage.
Teeth #7, #8, #9, and #10 were extracted without difficulty and a horizontal incision was done from #7-#10 placing 2 cc’s of cancellous particulate allograft condensed securely with an amalgam packer into the bony defect areas. Six single sutures were placed and post-operative instructions were given, including not to floss under the temporary bridge with normal brushing and flossing all other areas. See x-ray taken with bone graft in place.
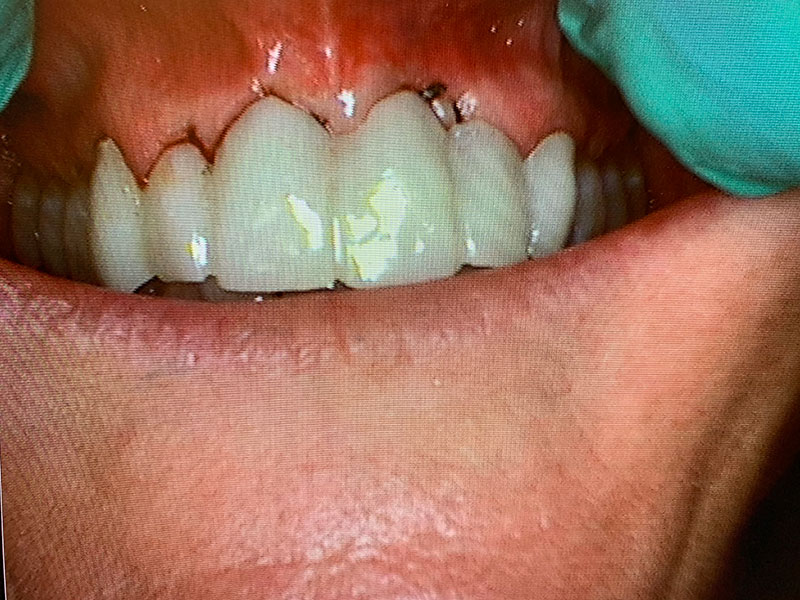
Temporary
When doing immediate crown and bridge, we envision the end product before beginning. In doing so we either wax up a model or use denture teeth in the edentulous area. This is after cutting out the teeth just like your lab would do for you if you sent it to the lab; then we make a stent for the temporary.
We usually do this in-house, but occasionally we send this out to a lab. The emergence profile of the bridge's pontics are key to a successful result. The patient was adamant not to have a “long tooth or teeth.”
Also, the ability to clean under the bridge keeping debris out is always better with a wider ridge. Of interest, we generally make the temporaries look good but not too good. Why? The patient will want to return for their long-term prosthesis! The long-term prosthesis is always smoother and looks better. The patient is generally thrilled with the final result and happy to “get rid of” the temporary. Some offices will have professional temporaries pre-made, and this is certainly acceptable. I found doing this raises the patient’s expectations and they anticipate the final restoration to be much better than the temporary. If this is not the case, the patient generally is unhappy. Remember, happy patient, happy life…or is that happy wife, happy life? Well, in actuality both of these sayings are so true!

Final
The ridge and emergence profiles were created so that the temporary can create a nice ridge lap appearance. See intraoral photo with temporary in place. It is important that the temporary creates the proper contours and profile prior to the final restoration being seated.
The temporary for immediate bridges after extractions and bone grafting is left in place for 6 weeks at a minimum. Once the patient has healed and the stability of bone height is noted we will lute the long-term prosthesis. I have found by doing this method for decades, the process works very well and the ridge does not shrink once the long-term prosthesis is placed. This is as long as the long-term prosthesis fits properly against the tissue and the bone graft is successful at the 6 weeks follow up. See the final cementation of long-term bridge #6-#11.
About Dr. John Dovgan: Dr. Dovgan has been retained by both Defendants’ and Plaintiffs’ counsel as an expert in the area of dental standard of care, and has been a continually practicing full-time dentist for over 30 years in Phoenix, Arizona. Dr. Dovgan is a board-approved consultant for over 25 years, adjudicating more than 1300 dental board cases for the State of Arizona.
Dr. Dovgan is contracted as the dental expert witness for the class action lawsuit in the State of Arizona (Parsons v Ryan), the class-action lawsuit in the State of Michigan (Johannes v Heyns) and for the Federal case Smego v. Mitchell in Illinois. Dr. Dovgan has been retained as a dental expert witness in over 150 malpractice cases throughout the United States since the beginning of 2010 due to his expertise in the standard of care. He currently has over 3,500 hours of continuing education, including advanced training in prosthetics (both removable and fixed), dental implants, risk management, occupational safety and health administration (OSHA), computer-aided design (CAD/CAM), cone-beam computer tomography (CBCT), full mouth reconstruction, lasers (both hard and soft tissue), and oral conscious sedation.

Dr. John Dovgan
Furthermore, Dr. Dovgan still currently consults and provides expert reports to the Arizona State Board of Dental Examiners developing the only board-approved template for appropriateness of care used by dental consultants and board members as well as the only preapproved online lecture for risk management for remediation in Arizona and New Jersey.
Dr. Dovgan has lectured and done live patient demonstrations using both hard and soft tissue lasers as well as having been published in restorative implant dentistry.
Lastly, Dr. Dovgan is a board-approved anesthesia evaluator and onsite inspection evaluator administering oral examinations and onsite inspections for 1303 anesthesia permits in Arizona.




