By Josh Bernstein, DDS
This very nice 55-year-old male ophthalmologist was referred by his orthodontist to solve a bite issue after undergoing jaw advancement surgery to successfully treat sleep disordered breathing. He had previously self-referred to a well-regarded university sleep clinic but had pursued surgical treatment without the guidance of an orthodontist. After surgery, his teeth no longer occluded.
Post-surgery, the patient developed a painful neuropathy that made even prophylaxis excruciating, and he had become resistant to local anesthesia, with resultant high fear of all but the most minor dental treatment. For these reasons, sedation was indicated.
Full mouth reconstruction was prescribed to re-establish occlusion. Occlusal analysis was performed to determine an ideal cranio-mandibular relationship, and that position was recorded. A full mouth diagnostic wax-up was ordered from a qualified dental laboratory technician.
Moderate IV sedation was indicated to perform the preliminary periodontal maintenance as well as for the preparations and cementations for full mouth reconstruction.
Pre-sedation physical determined the following:
- Patient is a healthy, fit, lean, muscular 55 year-old male.
- Height 5’8”, 170 lbs, BMI = 26
- No underlying medical conditions aside from post-surgical neuropathy and resistance to local anesthesia.
- Patient takes testosterone.
- Mallampati Class 3.
- ASA Class 1.
- Pulse oximeter readings were BP = 133/90, HR = 87, SPO2 = 95.
- RR = 12.
- Informed consent discussion initiated regarding risks, benefits and alternatives to sedation and restorative treatment. Pre-op and post op instructions were given, with particular emphasis on NPO status and obtaining a responsible adult companion for transportation and post op home care. Consent forms were signed and witnessed.
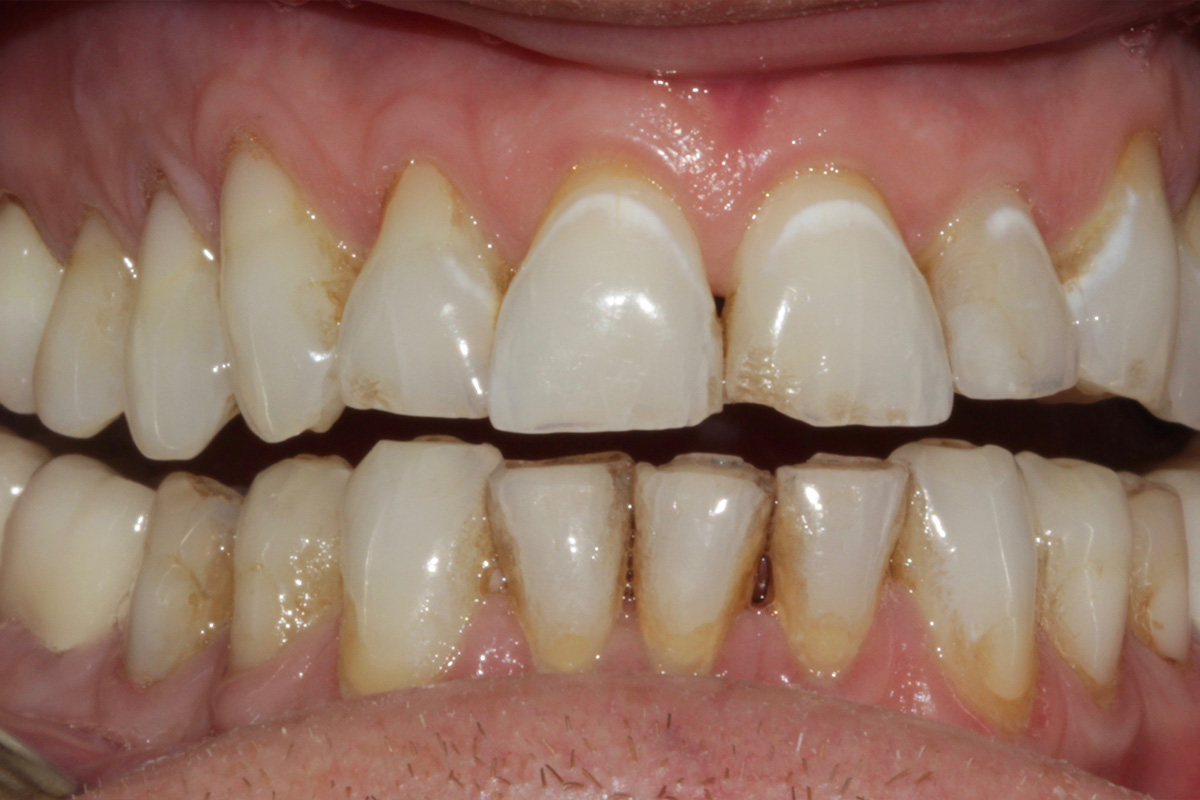
Pre-op retracted view: uppers and lowers
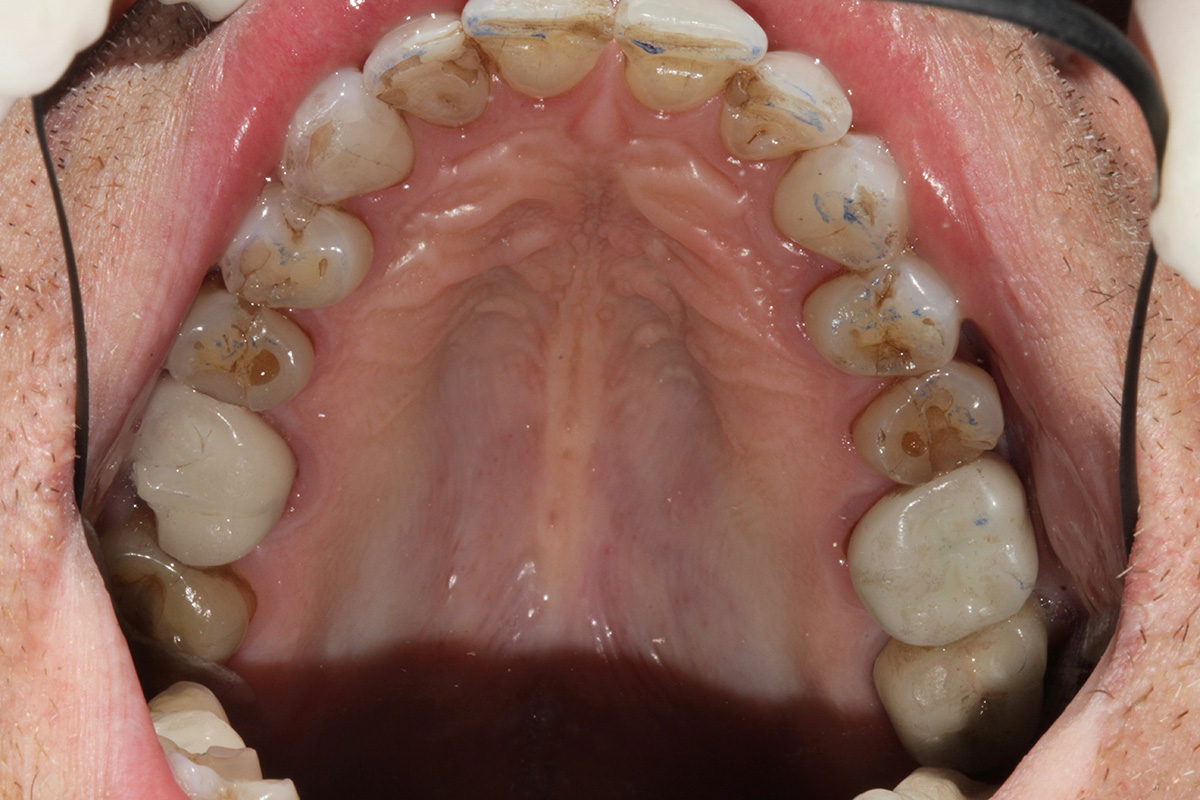
Pre-op: upper arch
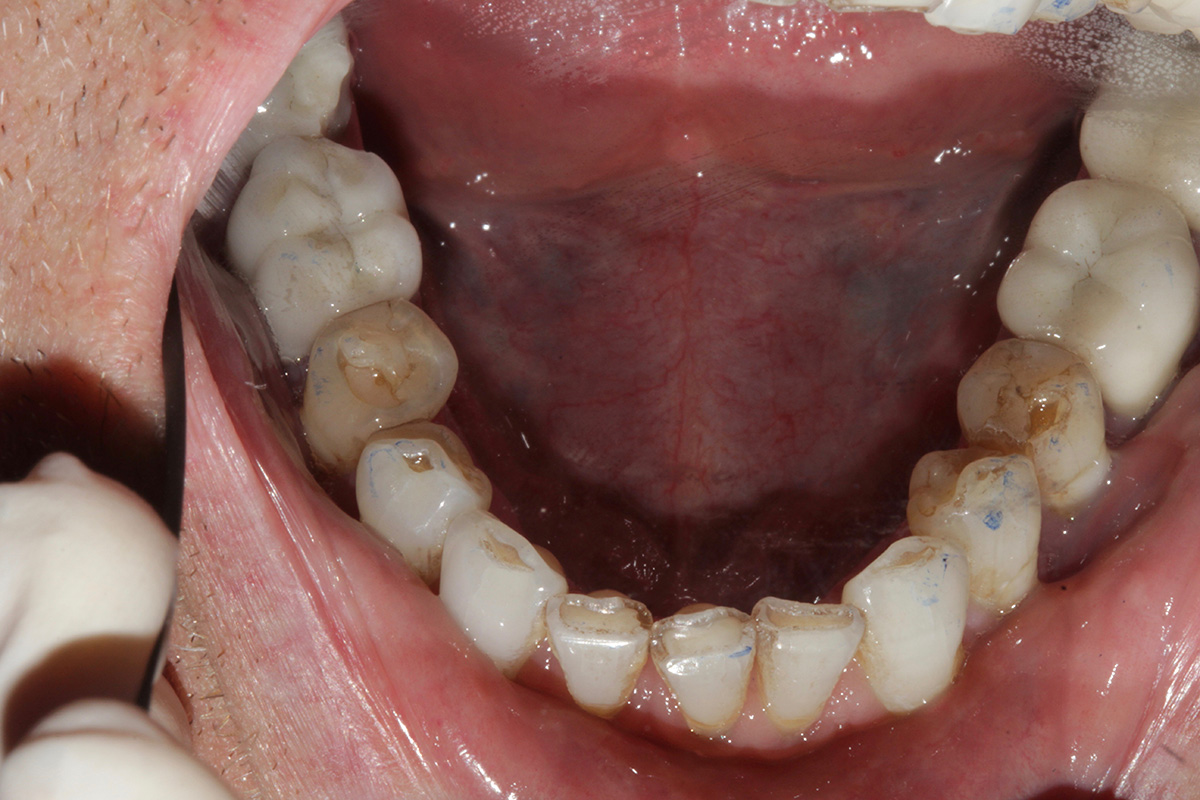
Pre-op: lower arch
Five sedation visits were required to complete treatment:
- Periodontal maintenance.
- Prepare uppers.
- Seat uppers.
- Prepare lowers.
- Seat lowers.
Post op visits were performed without sedation and were well tolerated by the patient.
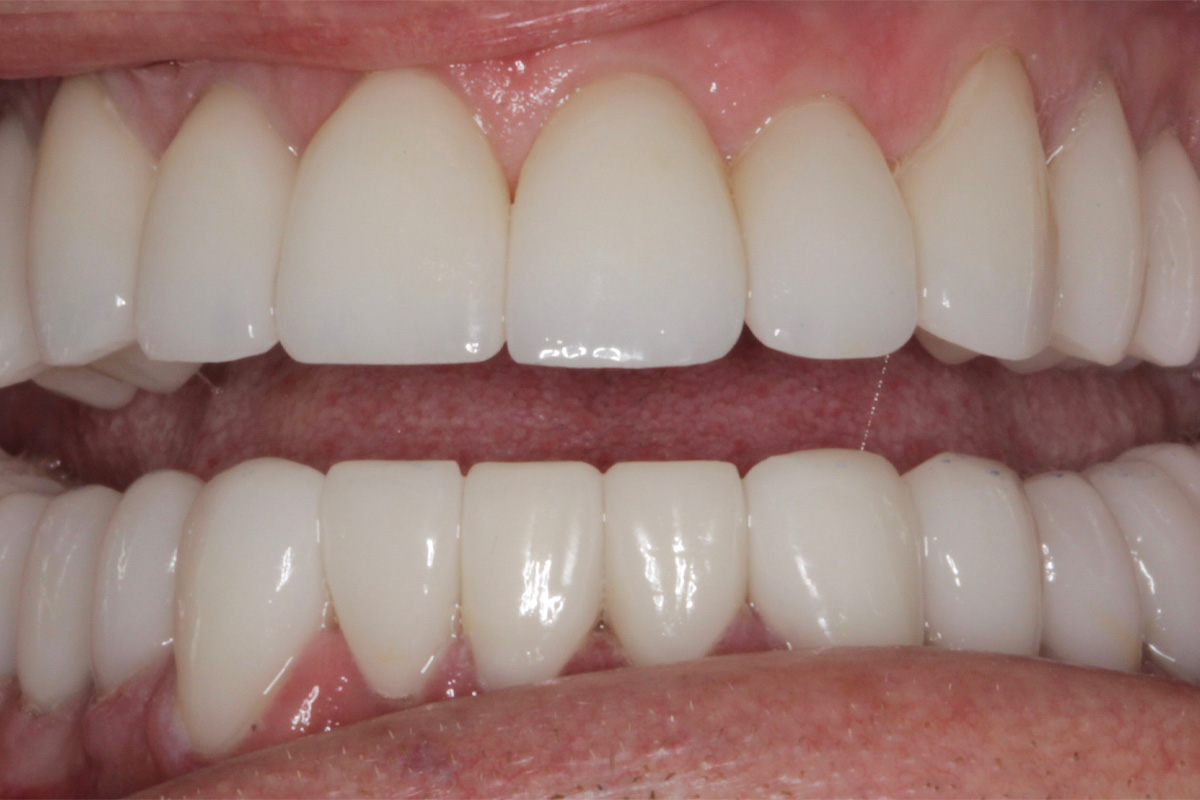
Post-op: uppers and lowers
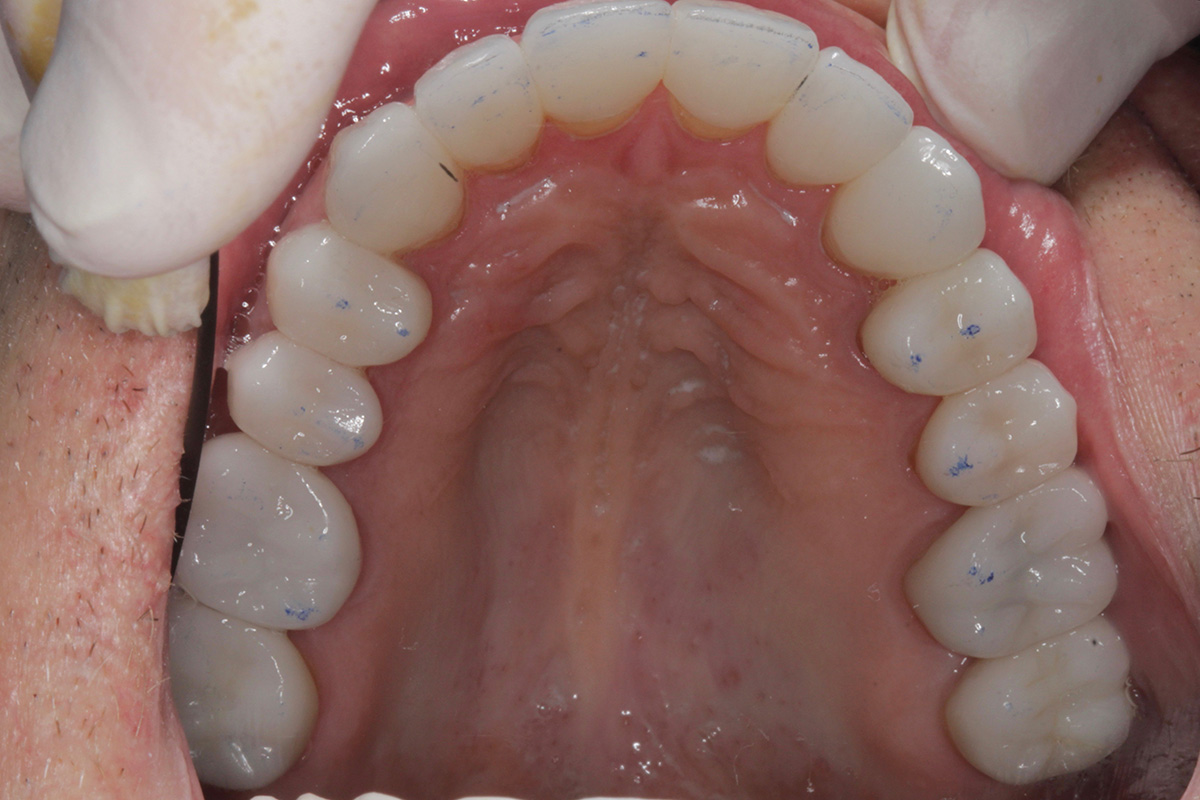
Post-op: upper arch
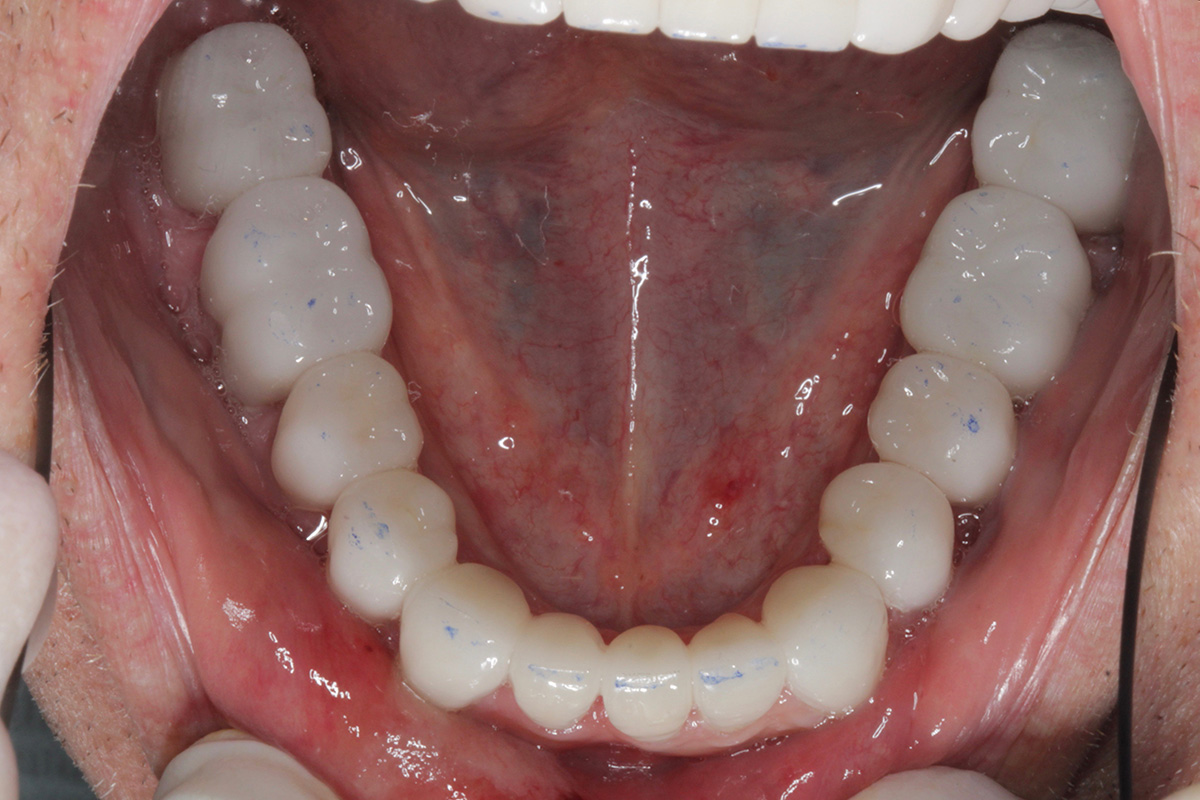
Post-op: lower arch
At each sedation visit, patient was compliant with NPO status and with securing a responsible adult companion for transportation and post op home care.
Upon arrival at each sedation visit, patient was encouraged to void before being seated. NPO status and post op companion were confirmed. Pre-op vitals were taken with a pulse oximeter which was left in place for the duration of each procedure. Patient was not-fearful of needles so no pre-sedation P.O. medication was required or given.
Venipuncture was established with a 22-gauge introducer on the right dorsal hand. IV tubing was attached from a 500 cc bag of lactated ringers + 5 % dextrose and adequate flow was confirmed without infiltration.
Two liters/minute of oxygen was administered from a nasal cannula and tubing was attached to a capnograph.
IV medications were titrated to effect for moderate sedation using midazolam, hydromorphone, and diphenhydramine. Articaine was used for local anesthesia. Additional medications were added periodically as needed, particularly during the longer preparation appointments, but they were not needed for the shorter periodontal maintenance visit.
The patient tolerated the procedures well; was alert, ambulatory and in good condition upon discharge to his companion with verbal and written post-op instructions. Patient was advised to take a combination of ibuprofen and acetaminophen for post-op analgesia as needed every 6 hours with food.
Using this protocol, this fearful, hypersensitive patient was able to undergo extensive dental treatment in complete comfort and relaxation. Proper occlusion was re-established, and his esthetic requirements were exceeded. The patient was very pleased with his treatment and with the final result.

Dr. Josh Bernstein maintains a fee for service, out-of-network private practice in Oakland, California, focusing on Cosmetic Dentistry, Sedation Dentistry and Invisalign. He is a Clinical Instructor in Cosmetic Dentistry, Full Mouth Reconstruction and IV Sedation. He serves as a Conscious Sedation Evaluator for the Dental Board of California. Dr. Bernstein lectures throughout the United States and is widely published nationally and internationally. Dr. Bernstein can be reached at [email protected]
Case study is written and printed with permission from Dr. Josh Bernstein. The porcelain was done by Bob Clark of Williams Dental Lab in Gilroy, California.




