We’re well into September, and that means flu virus season has arrived! But lurking in the shadows are ever-evolving coronavirus variants and growing concerns over the monkeypox virus.
By Genni Burkhart
At the time of this article, the Centers for Disease Control and Prevention (CDC) reports there’s a total of 21,985 monkeypox (MPX) cases in the United States with 57,995 cases globally. While the CDC website reports zero deaths in the US, the first confirmed death from MPX in the U.S. was reported on September 12th in Los Angeles County, California, with another potential death in Texas under investigation. The rapid increase of MPX led the Biden administration to declare the virus a “public health emergency” on August 4th.
Originally, MPX was primarily confined to African regions but has since spread to more than 88 countries including North America, Europe, and Australia. As the World Health Organization (WHO) declared the monkeypox outbreak a “Public Health Emergency of International Concern” back in July of this year, we’ll review the latest information available on MPX and its potential impact on dentistry.
First, Diligence
Weary as we all might be from the COVID-19 pandemic, we’re again reminded that continued due diligence is imperative in preventing the spread of contagious viruses, be it the seasonal flu, coronavirus variants, or monkeypox.
After the pandemic, already strict infection control practices dental practices follow became even more rigorous. The silver lining here might just be that dentists who are already following COVID-19 prevention procedures won’t really need to change their response for MPX.
A Note of Caution

While data suggests a specific segment of the population accounts for a majority of the current cases, anyone – regardless of age, gender, or sexual orientation – who has close personal contact with someone who has MPX, is vulnerable.
As reported in a July article on Today’s RDH the author Spring Hadfield, RDH BSPH states, “I want to caution health care professionals from stigmatizing this virus as a sexually transmitted disease that affects one group of individuals.”
Media reports have focused on the virus predominately afflicting homosexual men, but as Hadfield points out, this is the same bias that plagued the fight against HIV/AIDS, as many people refused testing and treatment for fear of being stigmatized. The MPX virus has not sought to infect one section of the population at a higher rate, rather the only true requirement “is to be a vertebrate.”
What to Look For
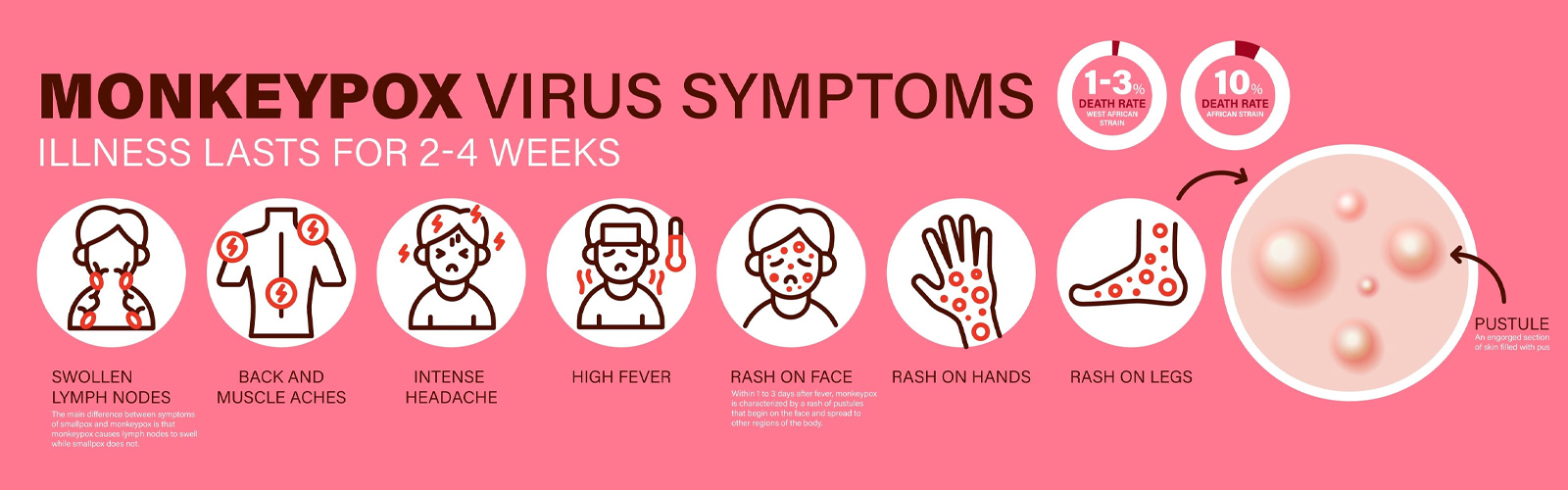
The CDC is reminding health care professionals to be alert for symptoms of MPX including oral lesions and referring those patients for further testing. Additional symptoms include rashes on the face, body, and inside the mouth, fever, headaches, body aches, swollen lymph nodes, respiratory congestions, fatigue, exhaustion and chills, sore throat, runny nose and cough.
MPX is part of the Orthopoxvirus genus in the family Poxviridae, the same family that causes the smallpox virus. Given that, symptoms of MPX are similar to smallpox symptoms, but (thus far) have shown to be milder and less fatal.
What Dentists and Hygienists Can Do
As stated, continuing to follow the same protocol for COVID-19 infection control will aid in protecting against the spread of MPX in the dental environment. Ana Karina Mascarenhas, B.D.S., D.Ph., chair of the ADA Council on Scientific Affairs stated in an article by Mary Beth Versaci on ADA News that "Dentists have provided care using standard infection control precautions for several decades now, and the enhanced protocols implemented during the COVID-19 pandemic will continue to keep our patients and staff safe during this monkeypox emergency. She continues, “Use of appropriate PPE including masks and gloves, surface cleaning, and extra diligence when examining patients for symptoms and the characteristic facial rash and intraoral lesions to identify a patient early are imperative."
For additional reference, the WHO released the “Clinical Management and Infection Prevention and Control for Monkeypox” rapid response guidance for health care facilities that you can download here. Specifics include:
- Contact and droplet precautions be implemented for any suspect patient with MPX. In addition to contact and droplet precautions, airborne precautions should be implemented if varicella zoster virus (i.e., chickenpox) is suspected and until it is excluded.
- In addition to contact and droplet precautions, respirators should be used.
- At the first point of contact with the health system, screening and triage should be performed for all persons who present with a rash and fever or lymphadenopathy.
In Conclusion
The MPX virus is still evolving, as is what’s known about this specific outbreak. For the most updated information on this virus, dental practices should make a regular habit of checking the CDC website.
The CDC suggests healthcare providers screen all patients for MPX and refer those who are suspected of having MPX for further testing. It’s also recommended that anyone who’s been exposed to MPX or is at higher risk of exposure to get vaccinated. Currently, there are two vaccines available to prevent MPX, but no specific treatment for the virus. However, antiviral drugs developed for smallpox can be used to treat MPX.
As stated by the American Dental Association (ADA), dental practices should continue to use the infection control precautions they’ve enhanced due to the COVID-19 pandemic to best protect staff and patients from MPX. What dentists shouldn’t do is stigmatize this virus and focus on any one particular population of patients. Rather, see this virus as the equal opportunity employer it truly is, with the potential to infect anyone regardless of age, gender, or sexual orientation.
Author: With over 12 years as a published journalist, editor, and writer Genni Burkhart’s career has spanned politics, healthcare, law, business finance, technology, and news. She resides on the western shores of the idyllic Puget Sound where she works as the Editor in Chief for the Incisor at DOCS Education out of Seattle, WA.




