By Dimitrios Kilimitzoglou, DDS
Smithtown, N. Y.
A 55-year-old female patient presented for consultation with the chief complaint that her lower partial denture was very loose. She had a history of mitral valve prolapse, glaucoma, occasional sinusitis, moderate anxiety and non-insulin-dependent diabetes, and was assessed as ASA II. The patient is completely edentulous in the maxilla, with remaining teeth #23, 24, 25, 26 and 27. These teeth displayed severe caries and advanced bone loss of 90 percent with mobility, making them unrestorable. She had experienced recurrent infections on her lower teeth, with thin ridges and limited keratinized tissue.
It was advised that she obtain a CT scan in order to evaluate the need for ridge augmentation. Mini dental implants and a complete denture were discussed as well as an implant-supported fixed bridge. The patient opted for mini dental implants and a complete denture. The patient was highly anxious about the procedure and agreed to intravenous sedation. The treatment plan included fabrication of an immediate mandibular complete denture, extraction of teeth #23-27, placement of five mini dental implants and insertion of an immediate implant-retained mandibular complete denture under IV sedation.
Her remaining teeth were splinted temporarily and alginate impressions were taken for a mandibular scanning appliance. After reviewing the CT scan, the appropriate implants were selected and steps for fabricating an immediate mandibular complete denture were initiated. After the denture was fabricated, the patient was ready for her appointment.
Amoxicillin 1000 mg, ibuprofen 600 mg were administered PO. The patient rinsed with 0.12 percent chlorhexidine gluconate for 30 seconds. Her pre-operative vitals were as follows:
- Blood pressure 144/81 mmHg
- O2 saturation 98 percent
- Pulse 77 bpm
- Temperature 99.4°F
- Respirations 23 per minute
- Weight 120 lb
- BMI 21
Nitrous oxide was administered at 60 percent via nasal hood, and a dual nasal cannula was also used for capnography, and was capable of delivering 100 percent supplemental oxygen if needed. A 22-gauge indwelling catheter was used to gain IV access on the right dorsum of the hand. Midazolam 2.5 mg was administered followed by fentanyl 50 mcg. Then, adjunct medications were administered as follows: 4 mg dexamethasone, 0.1 mg glycopyrrolate, 2.5 mg metoclopramide in order to decrease excess salivation and to prevent nausea and swelling. Midazolam was administered periodically to ensure anterograde amnesia and maintain a moderate level of conscious sedation. Total midazolam used was 8 mg. Total fentanyl administered 87.5mcg. A total of 144 mg of lidocaine and a total of 0.072 mg of epinephrine was utilized for local anesthesia.
Teeth #23, 24, 25, 26 and 27 were extracted and the tissue was modified accordingly. Minimal flaps were utilized, and the implant surgery was performed. All implants were 3M MDIs with a ball attachment. Implants were placed at the following sites: Site #21 1.8 x 10 mm, O-ball and collar, site #22 1.8 x 13 mm, O-ball and collar, site #24 1.8 x 13 mm, MDI standard, O-ball and collar, site #26 1.8 x 13 mm, O-ball and collar, site #28 1.8 x 10 mm, O-ball and collar. Site #28 showed good stability, torqued at 25 Ncm. All other implants demonstrated excellent stability, and the implant was torqued to 40 Ncm. Chromic gut 3-0 simple interrupted sutures were used. Ondansetron 2 mg administered about 15 minutes prior to the end of the procedure to prevent nausea and vomiting. Nitrous oxide was discontinued after the surgical part of the treatment was completed. Final periapical films were taken. Soft reline was used on the denture. The fit was satisfactory.
Post procedure vitals: BP 137/73, pulse 73 bpm, O2 97 percent, respirations 21 per minute. Total fluids administered were 350 ml of 5 percent dextrose in water (D5W). Post-op instructions were given verbally to the patient’s husband and provided in a written format. A transport chair was utilized to assist the patient to her car.
At a follow-up visit the patient had no recollection of the treatment appointment and experienced dull discomfort for two days without swelling, bleeding, bruising or complications. The sites healed unremarkably. This patient was safely and comfortably treated, with the use of sedation central to a positive outcome.
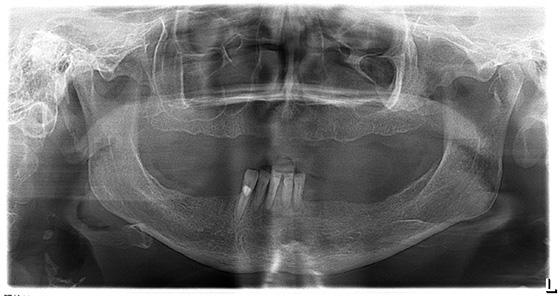
Before pano: Severely compromised lower aneriors.
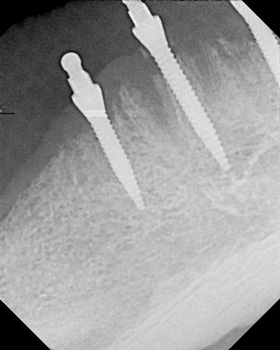
Post-placement healing at sites #28 and 26
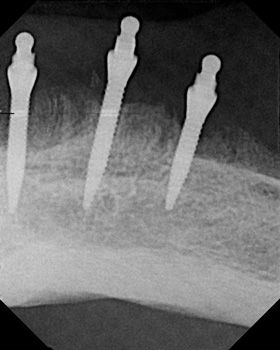
Post-placement healing at sites #24, 22, 21
Dr. Kilimitzoglou placing IV.
Dimitrios “Jimmy” Kilimitzoglou, DDS, DABOI, MAGD, FICOI, FAAID
Dr. Kilimitzoglou graduated from The State University of New York at Stony Brook School of Dental Medicine in 2012. He completed a two-year residency in Advanced Education in General Dentistry at SUNY Stony Brook, and also attended a one-year oral implantology program at the New York University College of Dentistry. Dr. Kilimitzoglou is a clinical associate professor at SUNY Stony Brook School of Dental Medicine, a fellow of the Long Island Academy of Odontology, and involved in dental implant research through the PEARL network at The NYU College of Dentistry. Dr. Kilimitzoglou is a major in the Air National Guard/Air Force, and a member of the 106th Medical Group, 106th Rescue Wing at Westhampton Beach, N. Y.
The information contained in this, or any case study post in Incisor should never be considered a proper replacement for necessary training and/or education regarding adult oral conscious sedation. Regulations regarding sedation vary by state. This is an educational and informational piece. DOCS Education accepts no liability whatsoever for any damages resulting from any direct or indirect recipient's use of or failure to use any of the information contained herein. DOCS Education would be happy to answer any questions or concerns mailed to us at 106 Lenora Street, Seattle, WA 98121. Please print a copy of this posting and include it with your question or request.




