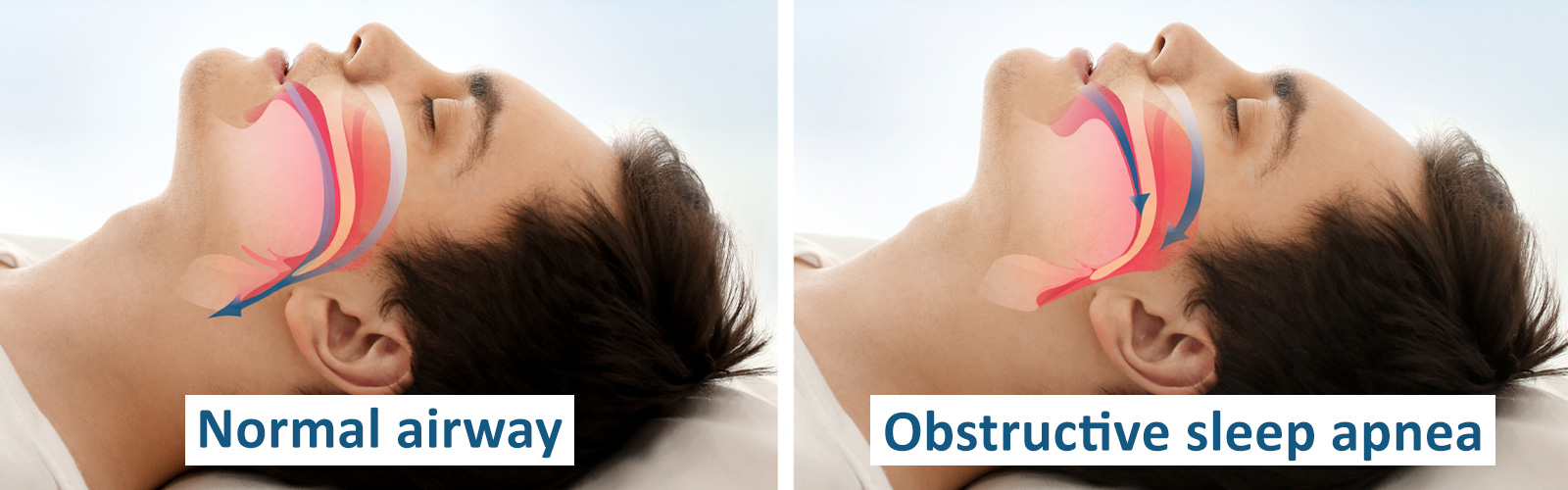
Sleep apnea can pose risks to patients undergoing dental sedation. To ensure patient safety, sedation dentists must be vigilant about sleep apnea and monitor patients effectively.
By Michael Silverman, DMD
Approximately 39 million Americans suffer from obstructive sleep apnea (OSA), of which 80% are undiagnosed and untreated.
During sedation, monitoring technology is similar to that used in sleep studies. Consequently, patients undergoing dental sedation may exhibit apneic events, temporarily cease breathing, and trigger the end-tidal carbon dioxide (ETCO2) alarm or a drop in the oximeter measurement below 90, signaling potential undiagnosed sleep apnea.
This is a significant concern for sedation dentists. Under dental sedation, sleep apnea, particularly in overlooked instances, can pose a serious health threat when the patient falls asleep.
Therefore, sedation dentists should be vigilant regarding sleep apnea, understand the safest monitoring procedures, and take steps to ensure the most effective care possible.
Undiagnosed and Untreated Sleep Apnea
During sedation dental procedures, patients are administered sedatives to help them relax and they often fall asleep. However, patients with sleep apnea are at an increased risk of complications during sedation due to the collapsible nature of their airway soft tissues.
Sleep apnea can lead to airway obstruction and decreased oxygen levels, which can have severe implications for dental sedation. Proper oxygenation levels are crucial during dental sedation and require a clear, unobstructed airway.
As such, using the STOP-Bang method, every dental sedation patient should be screened for sleep apnea during the health history pre-screening process.
It's then advised that dental patients with known sleep apnea only be sedated if a physician is successfully treating their condition.
Dental professionals should be aware of the potential risks associated with sedating patients with unknown or untreated sleep apnea. By pre-screening patients for the condition and ensuring that those with OSA are being medically treated, dental professionals can help minimize the risk of complications and ensure the safety of their sedation patients.
Treatment Precautions
Sedation dentists must take extra precautions when treating patients with sleep apnea, as they may be more sensitive to sedative and muscle relaxant agents.
Five steps to consider in treating apneic dental sedation patients:
- During the appointment, use 100% supplemental oxygen and consider using triazolam or midazolam for IV sedation. Longer-acting agents like lorazepam should be avoided, and diazepam should not be used the night before. Short-acting sedatives are preferred to minimize the risk of the patient being sedated at home without medical supervision. It's also best to reduce or avoid the use of analgesics with hypnotic action.
- Increased attention should be given to the position of the patient's airway.
- Because of the compromised airway, it's recommended to sedate the patient to a lighter level and avoid letting them fall asleep. If they do fall asleep, it's crucial to arouse them. Reversing them is acceptable if sleep apnea episodes are noticed.
- Patients requiring a full BiPAP are not candidates for sedation dentistry. Ask this question during the health history pre-screening process.
- It's imperative to avoid alcohol, muscle relaxants, and opioids. Opioids should not be prescribed for pain in these patients.
Patient Monitoring

Dr. Michael Silverman, DMD
When administering sedation to patients with sleep apnea, it is crucial to monitor their vital signs using reliable and trusted industry-standard equipment.
Intravenous (IV) sedation and enteral (oral) sedation should only be performed using a pulse oximetry device that measures heart rate, oxygenation percentage, blood pressure, and ETCO2.
The ETCO2 measurement is essential for monitoring a patient's airway during sedation and is the earliest indication of any potential breathing issues.
Monitoring ETCO2 levels is one of the latest care standards in sedation practice, while oxygenation is arguably the most important due to a need to maintain a high percentage of oxygenated hemoglobin. Monitoring ETCO2 has the advantage of alerting the practitioner of a cessation of breathing before the SpO2 measurement drops. Therefore, dental practices should invest in a high-quality monitoring device, such as the Edan X-10 or X-12, when practicing sedation.
These hospital-grade devices can print and digitally record heart rate, three-lead heart rhythm, ETCO2, and pulse oximetry every five minutes. It is worth noting that monitoring a patient's heart rate is essential in administering and monitoring sedative drugs throughout the appointment. Therefore, ensuring the monitoring technology is high quality and can provide accurate readings is crucial for sedation dentistry.
"As simple as it sounds, monitoring a patient’s heart rate is elemental in administering and monitoring sedative drugs." - Dr. Michael Silverman, DMD
Responding in Emergencies
Prevention is essential. However, in an emergency, the entire dental team must be prepared to assist immediately and effectively when necessary.
To determine if assistance is needed, you must first know the patient's tissue oxygenation and ventilation status.
If the pulse oximeter alarm sounds, indicating an undesirable level of oxygenation, the dental team should take the following steps in a logical series to correct the desaturation:
- Establish consciousness by asking the patient questions like, "Are you okay?" If the patient responds verbally, they are determined to be conscious.
- Open the airway by raising the chin.
- Check the equipment to ensure the finger clip is adequately positioned.
- Have the patient take a few deep breaths.
- Administer 100% supplemental oxygen.
- Reversal with flumazenil – 0.2-0.3mg or 2-3cc.
- Call for help by dialing 911.
The acronym for the steps to take when the O2 Saturation Alarm sounds is CAEBOR, which stands for Consciousness, Airway, Equipment, Breaths, Oxygen, and Reversal.
If the patient does not respond to verbal stimulation when the O2 saturation alarm sounds, then the above algorithm is modified to:
- Establish consciousness (patient is unconscious).
- Open the airway.
- Administer 100% supplemental oxygen.
- Reversal with flumazenil.
In Conclusion, Education and Preparation Remain Key
It's important to note that patients with sleep apnea may present some challenges for sedation dentistry. However, with proper education and preparation, dental professionals can provide these patients with safe and effective sedation.
It's crucial for the team first to be aware of the patient's medical history and any potential risks associated with OSA. Sedation dentists can ensure a successful and safe procedure for apneic patients by taking the necessary precautions and using high-quality monitoring technology.
Regular dental sedation education also reassures patients they're being looked after by a dental team that meets or exceeds dental sedation safety standards and regulations.
If you're not yet subscribed to receive the Incisor newsletter, filled with cutting-edge dental news sent directly to your inbox twice a month, you can do so here.
ABOUT THE AUTHOR
Dr. Silverman is a globally recognized lecturer, educator, author, and patient rights advocate and the founder and president of DOCS Education. He has appeared in front of 30 dental boards to advocate for dentists' right to provide sedation in an environment of safe and reasonable regulations. A graduate of the University of Pennsylvania School of Dental Medicine and believer in lifelong continuing education, Dr. Silverman continues to champion safe and effective minimal and moderate dental sedation.




