By Steven Tuggle, DMD
In 1895 Dr. Drotto Walkhoff forever changed dentistry in the same way that Professor Wilhelm Roentgen changed medicine a short time earlier. Roentgen used his wife’s hand and Walkhoff his own molars to take the first radiographs in medicine and dentistry. This first posterior dental radiograph took 25 minutes of x-ray exposure. While the quality was far from those seen on computer screens in dental offices today, it set dentistry on its pursuit of excellence in intraoral imaging.
Challenging this pursuit every step of the way has been the difficulty of balancing the need for patient safety and compliance with the dentist’s desire for the highest quality image possible. This conflict sometimes arises when deciding if the advantage of a cone beam CT outweighs the greater dose of radiation exposure or if a dental x-ray is necessary for the treatment of a pregnant patient.
An area of dentistry that is particularly dependent on high quality images is the diagnosis of interproximal caries. Diagnosing incipient interproximal caries can be challenging for the most experienced practitioner, whether looking at analog or digital images. Many clinical studies1,2 have shown no difference in conventional and digital radiographs’ accuracy in detecting interproximal caries and conclude that current imaging techniques have a low sensitivity for detecting carious lesions.
Shining a Light on OCT
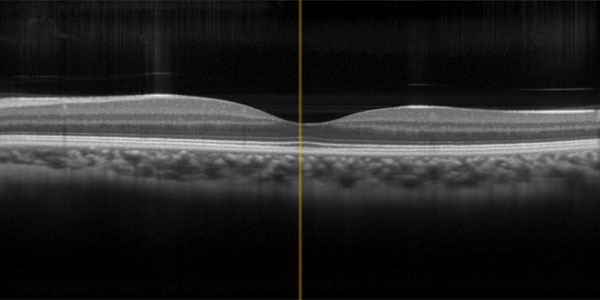
Image of an eye showcasing the same technology.
To view an example of a dental OCT, click here.
Facing the fact that dental caries affects 90% of the world’s population, dentists continue to research a more accurate and safer diagnostic imaging method. One of these methods is the use of optical coherence tomography (OCT)3,4. This is an emerging technology that utilizes light in the same way that an ultrasound uses sound for creating high-resolution cross-sectional images. Of great clinical dentistry significance in preventing cavitation of an incipient carious lesion is the fact that OCT accomplishes this on the micron scale and in real time.
Ophthalmologists use OCT to make cross-sectional images of the retina on the back of the eye. This enables inspection of each distinctive layer of the retina for a more accurate diagnosis. Cardiologists take advantage of OCT for high-resolution intravascular imaging which is becoming a tool in interventional treatment. Dermatology is also taking advantage of the benefits of OCT for skin diagnosis.
OCT offers several advantages for dentists in the diagnosis of interproximal caries of posterior teeth. A major obstacle dentists face when ordering radiographs is the patient’s resistance, citing the unnecessary exposure to dangerous radiation. OCT eliminates this problem by using non-ionizing radiation based on infrared light. This represents a major clinical advantage in treating pregnant patients and children.
Diagnosing with Reduced Risk
Dentistry has always taken pride in its research, teaching, and implementation of preventive and minimally invasive dental care. Clinicians often see a “spot” on a dental x-ray and are not sure if it is a carious lesion. This presents the dilemma of waiting and watching or placing a restoration immediately.
Both options come with a risk. If you watch and wait, a “spot” can turn into a carious pulp exposure before you have another opportunity to examine the tooth. On the other hand, no dentist likes drilling into a tooth, only to find nothing but sound and solid tooth structure. There is a need for a diagnostic tool to aid the dentist in detecting non-cavitated dental caries. This would allow dentists to initiate a protocol to arrest the caries and allow the patient’s tooth to remain intact.
OCT goes a long way toward meeting this goal. Professors Shimada and Yoshiyama4 studied the use of OCT in diagnosing interproximal caries on 51 proximal surfaces of 36 molars ex vivo. Each tooth received a score based on the degree of caries cavitation that ranged from sound tooth surface to a distinct cavity visible within the dentin.
OCT produced three-dimensional images that allowed for a detailed examination of each slice produced. This 3D method offered the advantage over 2D imagery of eliminating all artifacts in the images. The net result was the clinician’s ability to precisely identify and locate a carious lesion within the tooth’s anatomy.
Thirteen experienced dentists compared the OCT images with digital radiographs. Statistical analysis of the results concluded that 3D OCT images showed significantly higher sensitivity than conventional radiography in diagnosing interproximal caries.
There are still some challenges with the clinical application of OCT, such as the current inability to visualize the tooth's pulp chamber. However, with its great advantage of not exposing patients to ionizing radiation, OCT is sure to be a useful imaging methodology in the future of minimally invasive dentistry.

Author: Dr. Steven Tuggle received his DMD from the Medical College of Georgia before practicing general dentistry in the United States Navy. He then completed a residency in endodontics at the Medical College of Georgia. He recently retired from full-time practice limited to endodontics.
- Diagnostic Value of Conventional and Digital Radiography for Detection of Cavitated and Non-Cavitated Proximal Caries
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5557993/ - Comparison of the Accuracy of Digital Radiography with Conventional Radiography and Visual Examination in the Detection of Permanent Teeth Interproximal Caries
https://www.scielo.br/scielo.php?pid=S1983-46322019000100318&script=sci_arttext - Use of optical coherence tomography for assessment of dental caries: quantitative procedure
https://onlinelibrary.wiley.com/doi/abs/10.1046/j.1365-2842.2001.00840.x - 3D imaging of proximal caries in posterior teeth using optical coherence tomography
https://www.nature.com/articles/s41598-020-72838-2




